Our maternity service offers three birthplace options:
- Active Birth Centre
- Obstetric-Led Delivery Suite
- Home birth
Midwife-led antenatal clinics have resumed at the Midwife-Led Unit in the Mater Hospital. However, women who choose a midwife-led care birth will be accommodated at the Active Birth Centre in the Maternity Hospital.
If you have any queries about your Midwife-Led Unit clinic appointment, please contact the Mater Hospital antenatal team on 028 9504 1288.
We wish to reassure women that we will continue to offer and support midwife-led births in the Maternity Hospital.
We are here to support you and we are very grateful for your flexibility and understanding.
Active Birth Centre
The Active Birth Centre (ABC) is on the first floor of the Maternity Hospital. It has four birthing rooms:
- Sanctuary
- Serenity
- Harmony
- Haven
Each birthing room has an en-suite shower room and one has a fixed birthing pool.
The Active Birth Centre provides midwife-led care during labour and birth to women at low risk of complications.
Women with certain conditions may be supported to give birth in the Active Birth Centre. In this case, an individual care plan will be developed in partnership with you.
Download the Active Birth Centre leaflet.
Obstetric-Led Delivery Suite
The Obstetric-Led Delivery Suite is also on the first floor of the Maternity Hospital. It provides midwifery and obstetric care and has 12 birthing rooms, including a birthing pool.
The main delivery suite also has a dedicated obstetric operating theatre.
Home birth
If you live in north, south or west Belfast and are healthy with a straightforward pregnancy, you can have your baby at home.
Your community midwife can answer any questions you may have and discuss your home birth plans with you.
-
Induction of Labour
Labour is a natural process that usually starts between 37 and 42 weeks of pregnancy.
What is induction of labour?
This is a process that stimulates childbirth.
When will induction happen?
You may be offered an induction of labour:
- if labour has not started on its own you will be offered an induction of labour from 7 days after your expected date of confinement/delivery
- if the membranes have ruptured (waters have broken) but uterine contractions have not started and you are over 37 weeks pregnant
- if medical staff advise it’s needed due to concerns about your health or the health of your baby
Where will induction take place?
Your induction will take place in A ward of the Maternity Hospital. This is on the first floor.
How will my labour be induced?
You will meet the induction of labour team prior to your induction and a personalised plan will be agreed.
We use various methods of induction tailored to your requirements. These include:
- a cervical ripening catheter (foley catheter or balloon)
- artificial rupture of membranes (ARM)
- intravenous infusion of syntocinon (artificial hormone)
How long will induction take?
Inducing labour can take anything from a number of hours to a number of days.
Where is the induction of labour team based?
C ward
First floor
Royal Jubilee Maternity HospitalTel: 028 9615 0548
Mobile: 078 9533 1749To find out more information about the Induction of Labour click here.
-
Start of labour
There are several signs that labour is starting, but these can vary from woman to woman.
Signs that labour may be starting include:
- backache
- membranes rupturing (waters breaking)
- regular painful contractions – one contraction every five minutes.
Download our leaflet on coping with the very early stage of labour.
Some women experience backache, cramps or irregular contractions for several days or weeks before established labour starts. Contractions lasting a few hours are common and normal.
If you think you may be in early labour, call your community midwife or the Admission Assessment Unit for advice. False alarms are common with first time mothers.
This video by the Getting Ready for Baby team offers advice on how to cope with early labour at home:
If you are not in established labour when attending the Admission Assessment Unit, you may be advised to go home and wait for established labour (a regular pattern of painful contractions).
If you have your maternity records, please remember to bring them with you.
The area at the front of the maternity unit is a drop-off area only. It must be left clear for ambulances. There is a car park on the Royal Hospitals site opposite the Maternity Hospital.
When you arrive at the maternity unit, please give your name to the receptionist. You will then be assessed to check if labour has started and we will discuss choices for your baby’s birth.
It is essential that you bring a list of any medicines or tablets you may be taking. You should only take medicines prescribed by medical staff.
Please leave money and valuables at home with relatives. The maternity unit does not accept responsibility or liability for these.
If your birth experience is normal and uncomplicated, you will go home as soon as your condition allows and you may not need to stay overnight.
-
Delivery suite
When labour is established, you will normally be transferred to the delivery suite where you will be allocated a single room. Each room is pleasantly decorated and comfortably furnished.
A midwife will stay with you throughout your labour. She will care for and advise you during labour and assist with the birth of your baby.
Your partner or a person of your choice may stay with you during labour. The same person should remain with you throughout your stay in the delivery suite.
It is difficult for us to accommodate other visitors in the delivery suite as waiting facilities are limited. You may bring books, magazines and music with you. Throughout labour, you and your baby’s wellbeing will be monitored by the midwife.
-
Pain relief in labour
There are several ways of coping with pain and these are discussed at the antenatal education sessions. During labour, your midwife will be able to advise on pain relief in line with your needs.
- A birthing partner is a great help. They can provide emotional and physical support.
- Relaxation is important. A warm bath will ease backache and help you relax.
- It often helps to move around and adopt different positions.
- Transcutaneous Electrical Nerve Stimulation (TENS): This is a gentle electrical current passed through four contact patches applied to your back. It has no harmful effects and you can control the strength of the current yourself.
- Entonox (gas and air): Entonox is made up of 50 per cent oxygen and 50 per cent nitrous oxide. You inhale it through a mask or mouthpiece that you hold yourself. It is a simple process that acts quickly and wears off in minutes. It will not stop the pain completely but it may help.
- Morphine: This is a pain relieving injection given by a midwife that can make you drowsy and relaxed.
- Remifentanil: This is a pain relieving, intravenous drug controlled by a handset that you operate.
Click here to download and read the Remifentanil leaflet. - Epidural: This is an effective method of pain relief where a fine tube is inserted into your back and pain relieving drugs are passed through it. It is recommended for long labour or particular pregnancy complications.
-
Positions for labour
No one knows for sure which position is best for you and your baby when you go into labour. The position you give birth in is up to you. The midwives will be able to assist you in your choice.
Being upright in labour
Being upright can generally help in the following ways:
- gravity could help your baby move down more easily and more quickly
- there is less pressure on the blood vessels that go to your womb – these provide your baby’s oxygen supply
- your contractions could work better, which helps you open up more quickly
- your baby could be in a better position for moving through your pelvis
- when you squat or kneel, your pelvis may open wider and make more room for the baby to come through
Researchers have looked at the advantages of being upright during the two stages of labour:
- first stage is from the start of contractions until you’re ready to push
- second stage is from when you start to push until the baby is born
First stage
Being upright during the first stage could mean standing, sitting, squatting, kneeling, using a birthing ball or walking around. The research compared these positions to lying down.
Advantages of being upright:
- it is less painful
- there is less need for an epidural or painkilling injection
- labour could be slightly shorter
Second stage
Being upright during the second stage could mean kneeling, squatting, sitting fairly straight.
Advantages of being upright:
- it is more comfortable and less painful
- pushing is easier
- there is less chance of having a suction cup, forceps or caesarean delivery
- there is less chance of getting an infection in your womb
- there is less chance of tearing your vagina or the skin between your vagina and anus
- babies stand a better chance of breathing well right after they’re born
- labour could be shorter
Disadvantages of being upright:
- there is more chance of tearing your labia (the lips around the vagina)
-
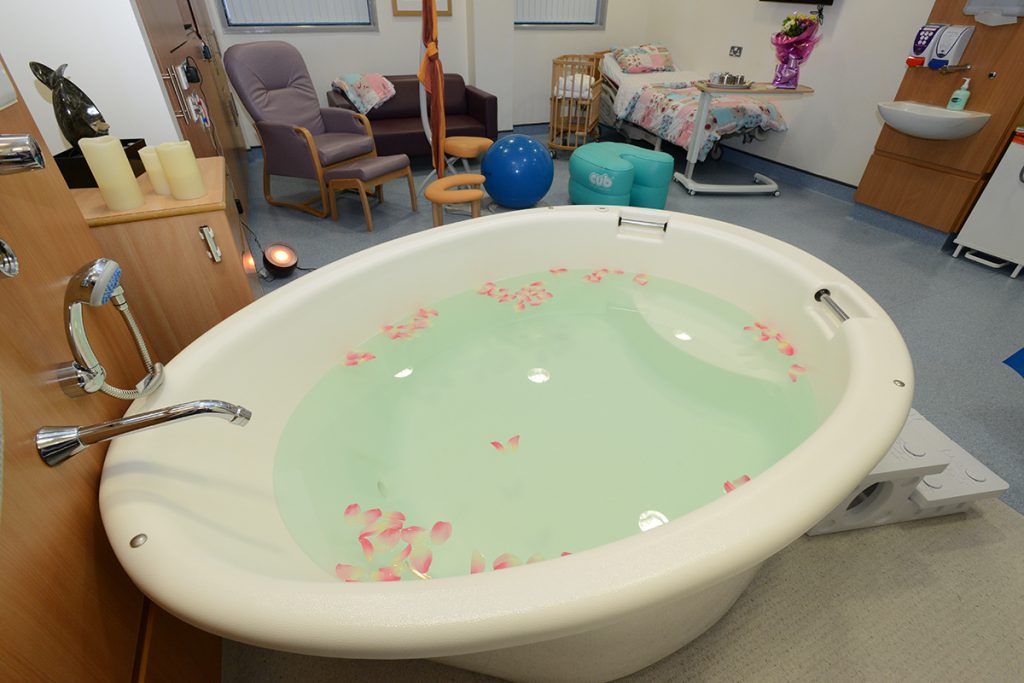
Birthing pools
We support the use of water for both labour and birth.
There are two pools in the Maternity Hospital – one in the delivery suite and one in the Active Birth Centre.
Women have commented on the relaxing effects of the birthing pools. The warmth and support of the water means many women require less pain relief and experience more effective contractions.
The pools also offer greater privacy and reduce the need for intervention. You can continue to use Entonox (gas and air) while in the birthing pool. During early labour, you might find it helpful to relax in your bath at home.
If you are interested in using a birthing pool, please ask your midwife for further information.
-
Ways to give birth
Normal birth
More than half of all births are normal, with the baby being born vaginally by maternal effort.
We aim to ensure that your birth preferences are followed, but there are times when things do not go according to plan. Therefore, we may need to make changes to ensure the safety of both you and your baby. If your baby shows signs of distress, the birth may require some assistance.
Assisted vaginal delivery
It may be necessary to assist the birth of your baby. This may involve a vacuum cup applied to the top of your baby’s head or forceps applied to each side of your baby’s head. Both of these instruments are used to enable delivery of your baby through the birth canal.
Caesarean section
Approximately one in four babies are born by caesarean section. This figure includes both planned and unplanned caesarean sections.
The decision to do a caesarean section will be taken by the clinical team. In most circumstances, a spinal or epidural anaesthetic is used. This allows you to be awake for the birth.
In the operating theatre, you will be cared for by a team of midwives, doctors and maternity support workers. After the birth, we will continue your care in the recovery suite before you are transferred to a postnatal ward.
Download our leaflet on preventing infection following caesarean birth.
-
Following the birth of your baby
Immediately after birth, your baby will be examined and weighed by your midwife.
Two identification bands with your baby’s details will be checked by the midwife together with you and your partner. One of these bands will be wrapped around your baby’s wrist and the other around the ankle. Both bands must remain in place until your baby is at home. Please inform your midwife if a band needs replaced.
Your midwife will check that you and your baby are both recovering well. Practical advice on caring for your baby will be offered. This includes information on feeding and nappy changing.
Your midwife will also encourage skin to skin contact between you and your baby.
Keeping your baby close (rooming-in)
Your baby will stay in a cot in the same room as you. Keeping your baby close gives you a chance to get to know each other. It also helps you gain confidence in caring for your baby.
You will learn to recognise your baby’s feeding signals and be responsive to their needs. Staying close also means you will notice any problem with your baby.